PERIODONTAL TREATMENT
Gingivitis
Gingival inflammation
Healthy gums typically exhibit a light pink hue and firm texture. However, individuals with a higher amount of melanin in their gums may have a darker pigmentation.
In contrast, red and swollen gums that bleed easily during brushing may indicate inflammation and the presence of gingivitis, a common form of gum disease.
This inflammation is often caused by the presence of plaque, a sticky film that forms along the gum line due to the presence of bacteria in the mouth. The toxins released by the plaque can irritate the gums, leading to inflammation.
In addition to microbial plaque, other factors can contribute to the appearance of periodontal disease.
These include:
- Systemic diseases (e.g. diabetes mellitus, hematological diseases, AIDS, etc.)
- Hormonal changes (e.g. diabetes, pregnancy, menopause etc.)
- Prescription drugs (e.g. antihypertensives, antiepileptics, contraceptives etc.)
- Smoking (smokers do not respond as well to the therapeutic effect)
- Malformed prosthetic restorations (bridges, crowns)
Effective daily oral hygiene at home, with proper brushing and flossing, together with regular visits to your dentist can help prevent this condition from progressing into periodontal disease, which can result in tooth loss if left untreated.
Gingivitis to periodontitis progression
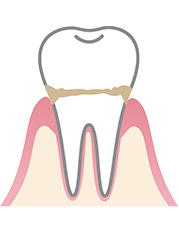
Gingivitis

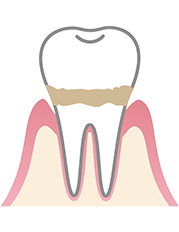
Early periodontitis

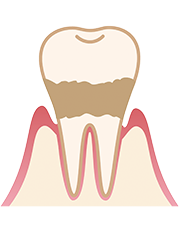
Moderate periodontitis

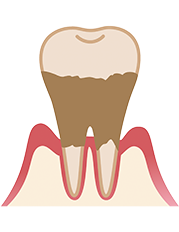
Severe periodontitis
Periodontal inflammation
Periodontitis is a chronic inflammatory disease that affects the gums and supporting tissues of the teeth. Without proper treatment, it can lead to tooth loss. The condition occurs when bacteria in dental plaque accumulates and progresses deep into the gum line, resulting in inflammation of the surrounding tissues and jawbone. Unfortunately, the supporting structures that are damaged due to periodontitis cannot regenerate, leading to loose teeth.
There are many signs that will make you suspect that you may be suffering from periodontitis such as:
- bleeding gums
- feelling of loose teeth
- receding gums
- bad breath
- feeling like your teeth have ‘moved’
There are many types of periodontitis and the most common type is chronic periodontitis where we see inflammation in the supporting tissues of the teeth and progressive bone loss.
In chronic periodontitis we also see pocketing (deepening of the gingival fissure) and loss of tissue attachment from the teeth.
Other types of periodontitis are aggressive periodontitis, periodontitis as a result of systemic diseases (general health), ulcerative periodontitis and periodontitis due to continuous trauma.
The main cause of periodontitis is the dental microbial plaque and its accumulation. However, there are many aggravating factors that contribute to the outbreak of the disease.
These include:
age, smoking, heredity, stress, certain medications,
“clenching” or “grinding” teeth, systemic general health conditions, malnutrition and obesity.
With the suitable treatment recommended by our team and adjustments made to any exacerbating factors, we can effectively manage periodontal disease.
In cases where non-surgical treatment is insufficient, surgical intervention may be necessary to restore gum and bone health.
During your initial visit, a comprehensive dental and radiographic evaluation will be conducted.
Additionally, the depth of periodontal pockets, attachment loss, and any other pathological observations of the periodontal tissues will be recorded.
After evaluating the severity of the periodontal disease, the appropriate treatment is initiated, which may include conservative root scaling and planing or surgical interventions, tailored to each patient’s specific case.
A follow-up review system is then implemented to closely monitor the progression of the disease or its restraint.
Scaling and root planning
What is it ?
Deep scaling or root planing is the process of cleaning the places between the gums and the teeth, thus, eliminating the disease-caused by the bacteria in them.
Essentially, we will will remove the tartar and plaque from gum pockets, promoting healing of the gums.
Process
Scaling and root planing is done with the use of ultrasonic scalers and hand instruments.
- First, ultrasonic scalers are used to remove larger deposits of plaque and tartar from the crowns and roots of teeth.
- Next, hand instruments called scalers and curettes are then used to remove any remaining deposits in the deeper pockets and to make sure the tooth surfaces are clean and smooth.
Additional antiseptic mouth rinse or antibiotics may be prescribed after the treatment to aid with the healing process.
The whole procedure may be done in a single visit, however, treatment per quadrant (one-fourth of the mouth) or per one-half of the mouth (right or left, upper or lower) is recommended per appointment especially for very deep pockets and extensive rough root surfaces since anesthesia will be used.
Healing
Ideally, after the deep scaling and root planing appointment, healing should be observed as long as it is coupled with the best daily oral hygiene measures.
After 2 weeks to 1 month, a reassessment can be done to check for changes in the gums such as the healing of the diseased gum pockets.
For periodontitis patients, more frequent visits to the dentist are a must to maintain the healthy state of the gums and to prevent the reformation of pockets.
A consistent oral hygiene routine of twice-daily tooth brushing and daily flossing is also needed to maintain a good oral health.
Laser assisted periodontal treatment
What is it ?
Scaling and root planing is a traditional treatment for periodontal disease. This procedure cleans the surfaces of teeth and their roots from plaque and calculus, which may be exposed due to gum recession.
The dental laser is an effective tool for the treatment of periodontal disease, and it can be used to treat both gingivitis and periodontitis.
Combining dental laser treatment with scaling and root planing can effectively treat periodontal disease. After removing dental plaque and calculus, the laser is used to remove infected tissue from the gingival pockets, eliminating periodontal microorganisms.
The laser emits high-frequency, low-energy light that targets specific cells such as bacteria or infected tissue without harming surrounding tissues, including the gums.
As a result, the procedure is safe and non-invasive.
BENEFITS
Laser therapy is not only effective but also has a number of benefits over traditional forms of treatment.
Treatment with a dental laser is non-invasive, tissue-preserving, and regenerative. The high-frequency, low-energy laser light helps to remove the bacteria and stimulate new tissue growth.
The use of a dental laser reduces postoperative bleeding, swelling, and pain. It also allows for faster healing time than traditional treatment methods.
In addition to the reduction in treatment time, it has been proven to be more effective than traditional scaling and root planing in reducing the amount of bacteria in the gingival pockets. This means that your dentist will be able to treat any infection at an earlier stage of development, preventing it from developing into a more serious problem.